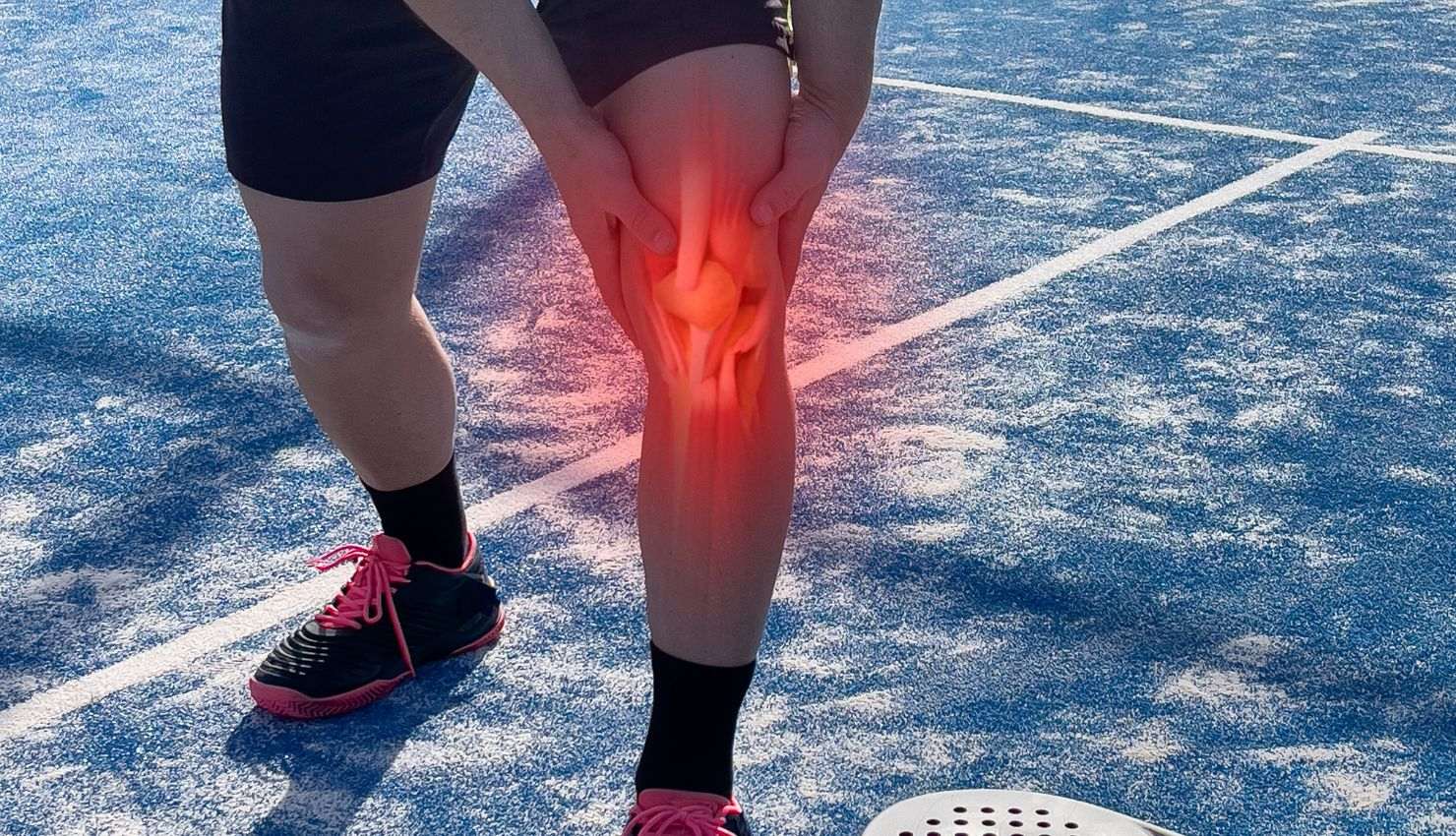
Bursitis is the inflammation of a bursa, a small, fluid-filled sac that cushions the bones, tendons, and muscles near the joints. This condition typically occurs due to repetitive motion, excessive pressure on a joint, or trauma, leading to swelling, pain, and limited mobility in the affected area.
Bursitis is the inflammation of a bursa, a small, fluid-filled sac that cushions the bones, tendons, and muscles near the joints. This condition typically occurs due to repetitive motion, excessive pressure on a joint, or trauma, leading to swelling, pain, and limited mobility in the affected area. Common areas affected by bursitis include the shoulder (subacromial bursitis), hip (trochanteric bursitis), knee (prepatellar bursitis), and elbow (olecranon bursitis).
Physiotherapy is a vital treatment for managing and alleviating the pain caused by bursitis. Physiotherapists use various techniques to reduce inflammation, restore joint mobility, strengthen muscles, and prevent future flare-ups. Heres how physiotherapists help with pain caused by bursitis:
### **1. Comprehensive Assessment and Diagnosis**
The first step in managing bursitis with physiotherapy is a thorough assessment. The physiotherapist will evaluate the extent of the injury, the underlying causes of the condition, and how it is affecting your mobility and daily activities.
#### **What Happens During the Assessment:**
* **Medical History**: The physiotherapist will ask about the onset of pain, previous injuries, repetitive movements, and activities that might have contributed to the development of bursitis.
* **Physical Examination**: The physiotherapist will assess the affected area for signs of inflammation, tenderness, swelling, and limited range of motion (ROM). They may also evaluate muscle strength, posture, and movement patterns to identify contributing factors.
* **Functional Assessment**: The physiotherapist may observe how the pain affects your ability to perform tasks such as lifting, walking, or bending to determine how bursitis is impacting your daily life and identify goals for rehabilitation.
Once the assessment is completed, the physiotherapist will develop a personalized treatment plan to address the inflammation, pain, and functional limitations caused by bursitis.
—
### **2. Pain Relief Techniques**
Pain management is crucial for the initial stages of bursitis treatment. Physiotherapists employ various methods to reduce pain and inflammation, enabling you to engage in exercises and activities that promote healing.
#### **How Physiotherapists Manage Pain:**
* **Cold Therapy (Cryotherapy)**: Ice packs or cold compresses are used to reduce inflammation and numb the pain in the affected area. Cold therapy is especially effective during the acute phase of bursitis, when swelling and irritation are most pronounced.
* **Heat Therapy**: Heat is applied after the initial inflammation has subsided. Heat therapy helps relax the muscles, relieve stiffness, and increase blood circulation to promote tissue healing in the affected area.
* **TENS (Transcutaneous Electrical Nerve Stimulation)**: TENS units use electrical impulses to block pain signals and stimulate the release of endorphins, the bodys natural painkillers, providing non-invasive pain relief.
* **Ultrasound Therapy**: Therapeutic ultrasound uses sound waves to penetrate deep into tissues, promoting blood circulation, reducing inflammation, and accelerating tissue repair in the affected joint.
These pain management modalities provide effective relief, helping to create a more comfortable environment for healing and rehabilitation.
—
### **3. Manual Therapy**
Manual therapy is a hands-on approach that can help reduce pain, restore mobility, and improve muscle function. Physiotherapists use specific manual techniques to address the discomfort caused by bursitis.
#### **How Physiotherapists Use Manual Therapy:**
* **Soft Tissue Mobilization**: Physiotherapists apply massage techniques to reduce muscle tension, alleviate discomfort in surrounding tissues, and improve circulation around the bursa. This can help reduce pain and promote healing.
* **Joint Mobilization**: For bursitis that involves restricted joint movement, physiotherapists use gentle joint mobilization techniques to improve the range of motion (ROM) and reduce stiffness in the affected area.
* **Myofascial Release**: This technique targets tightness and restrictions in the fascia (the connective tissue surrounding muscles) to release tension and improve tissue flexibility, helping to alleviate pain from bursitis.
Manual therapy helps reduce stiffness, improve joint mobility, and relieve the muscle tension that often accompanies bursitis.
—
### **4. Stretching and Flexibility Exercises**
Tight muscles and limited flexibility are often associated with bursitis and can exacerbate pain in the affected area. Physiotherapists use stretching and flexibility exercises to restore normal range of motion (ROM), alleviate tension, and reduce pain.
#### **How Stretching Helps with Bursitis Pain:**
* **Targeted Stretching**: Physiotherapists prescribe stretches that focus on the muscles surrounding the affected bursa. For example, if you have shoulder bursitis, stretches may target the shoulder and upper back to relieve tension and improve mobility.
* **Gentle Range of Motion (ROM) Exercises**: Passive or active ROM exercises are introduced to maintain or restore movement in the affected joint. This helps reduce stiffness and improve function while preventing the formation of scar tissue.
* **Dynamic Stretching**: Once the acute inflammation subsides, dynamic stretching can be introduced to further increase flexibility and prepare the affected joint for functional activities.
Stretching exercises help increase flexibility, reduce muscle tightness, and restore normal movement, which alleviates pain caused by bursitis.
—
### **5. Strengthening Exercises**
Weakness in the muscles surrounding the affected joint can exacerbate bursitis pain and lead to further injury. Physiotherapists incorporate strengthening exercises to improve muscle support and reduce strain on the bursa, promoting healing and preventing future flare-ups.
#### **How Strengthening Exercises Help Manage Bursitis Pain:**
* **Targeted Muscle Strengthening**: Physiotherapists prescribe exercises to strengthen the muscles around the affected joint, such as the rotator cuff for shoulder bursitis or the hip abductors for hip bursitis. Stronger muscles reduce the load on the bursa and provide better stability and support to the joint.
* **Progressive Resistance Training**: Strengthening exercises are gradually introduced, starting with low resistance and increasing as healing progresses. This ensures the muscles are strengthened safely without overloading the injured area.
* **Functional Strengthening**: Physiotherapists often incorporate functional exercises that simulate daily movements, such as lifting, bending, or reaching. This helps improve strength and joint stability, reducing the likelihood of further injury.
Strengthening exercises help support the joint, reduce strain on the bursa, and prevent future pain or injury.
—
### **6. Postural and Movement Education**
Poor posture and improper movement patterns can contribute to the development of bursitis or worsen existing symptoms. Physiotherapists assess your posture and movement habits to identify factors that may be exacerbating the condition.
#### **How Physiotherapists Address Posture and Movement:**
* **Postural Correction**: Physiotherapists educate you on maintaining good posture, especially during activities that put stress on the affected area (e.g., sitting, standing, or lifting). Proper posture reduces strain on the bursa and surrounding tissues, alleviating pain and promoting healing.
* **Movement Analysis**: Physiotherapists observe how you move during everyday tasks, such as walking, bending, or lifting. They identify any abnormal movement patterns that may be contributing to your symptoms and provide corrective exercises or tips to improve efficiency and reduce pain.
* **Ergonomic Adjustments**: For individuals with work-related bursitis (e.g., shoulder or elbow bursitis), physiotherapists recommend ergonomic adjustments to your workstation or tools to minimize repetitive strain on the affected joint.
Improving posture and movement habits reduces strain on the bursa and surrounding structures, helping to alleviate pain and prevent further injury.
—
### **7. Education on Self-Care and Prevention**
Physiotherapists play a key role in educating patients about self-care strategies that can help manage bursitis pain and prevent future flare-ups. This is an essential part of long-term recovery and pain management.
#### **Self-Care and Prevention Strategies:**
* **Home Exercise Program**: Physiotherapists provide a personalized home exercise program that includes stretching, strengthening, and mobility exercises to continue rehabilitation outside of sessions.
* **Pain Management**: Physiotherapists educate patients on how to manage pain at home using techniques like ice/heat therapy, rest, and proper body mechanics to reduce strain on the affected area.
* **Lifestyle Modifications**: Physiotherapists recommend lifestyle changes such as modifying activities, using supportive footwear, or incorporating rest days to allow the body to recover without overloading the affected joint.
By empowering patients with self-care tools and prevention strategies, physiotherapy helps individuals take an active role in their recovery and long-term well-being.
—
### **8. Long-Term Maintenance and Rehabilitation**
Once the acute pain from bursitis has been managed, physiotherapists focus on rehabilitation and long-term maintenance to prevent recurrence and support ongoing joint health.
#### **How Physiotherapy Helps with Long-Term Maintenance:**
* **Ongoing Strengthening and Flexibility**: Physiotherapists recommend continuing strengthening and flexibility exercises to maintain muscle support, joint mobility, and overall function.
* **Activity Modification**: Physiotherapists help you maintain an active lifestyle while avoiding activities that might strain the affected area. They may recommend low-impact exercises, such as swimming or cycling, to maintain fitness without exacerbating symptoms.
* **Regular Check-Ins**: Physiotherapists may schedule follow-up visits to monitor progress, address any emerging issues, and adjust the treatment plan as needed to ensure long-term recovery and pain-free movement.
By maintaining strength, flexibility, and healthy movement habits, physiotherapy ensures that you can continue to live an active life without the recurring pain of bursitis.
—
### **Conclusion**
Physiotherapy is an effective, non-invasive treatment for managing the pain caused by bursitis. Through pain management techniques, manual therapy, stretching, strengthening exercises, postural correction, and education, physiotherapists help individuals reduce pain, restore function, and prevent future flare-ups. By addressing the root causes of bursitis and promoting long-term joint health, physiotherapy allows you to manage your condition effectively and return to normal activities with minimal pain. If you are experiencing pain from bursitis, consulting a physiotherapist can provide the support and strategies necessary for a full recovery and improved quality of life.