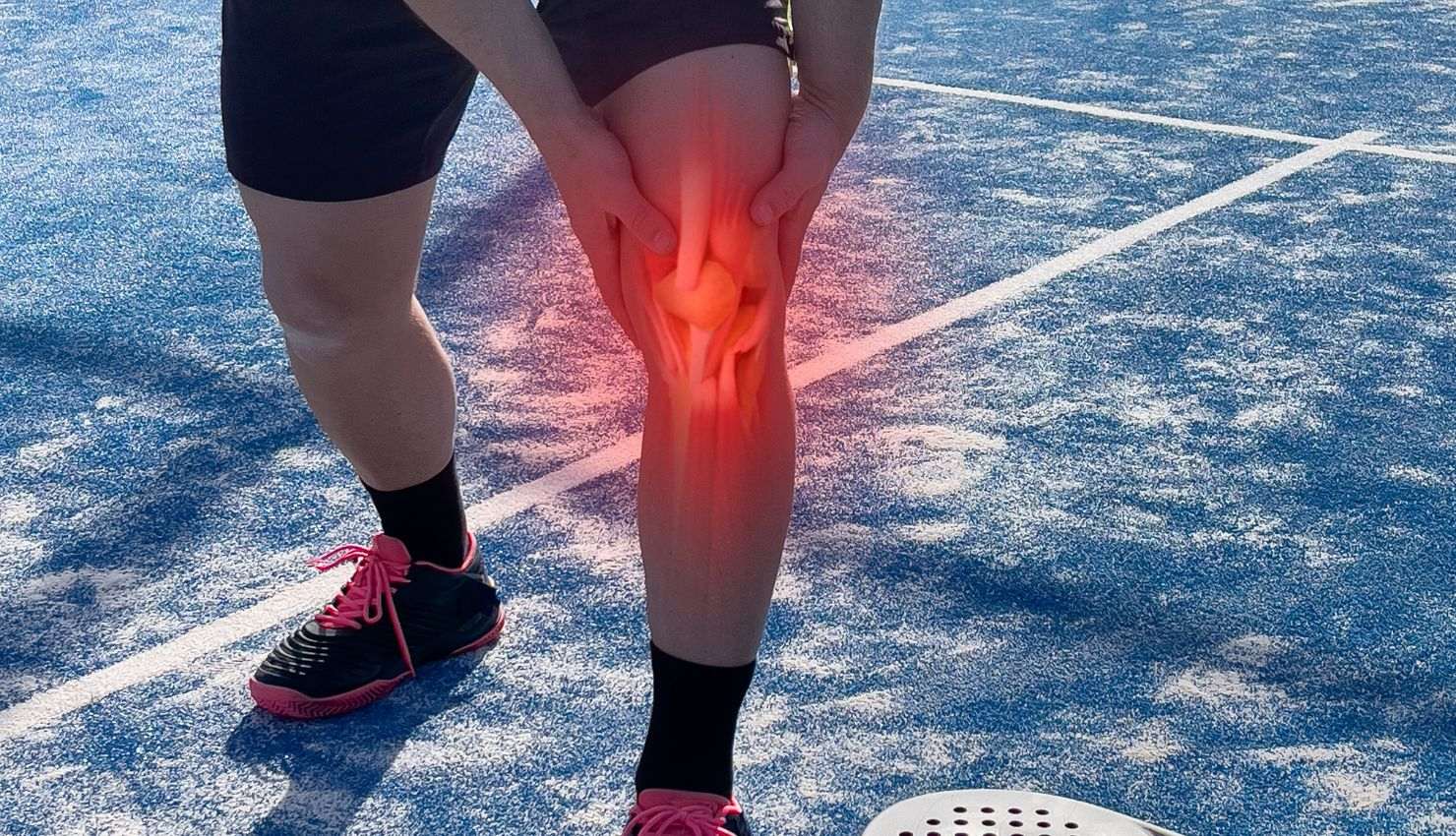
Surgery is controlled trauma to the body. The pain and swelling you feel are part of the bodys natural healing process: Pain often comes from tissue trauma, incisions, muscle tension, or nerve sensitivity.
Surgery is controlled trauma to the body. The pain and swelling you feel are part of the bodys natural healing process:
Pain often comes from tissue trauma, incisions, muscle tension, or nerve sensitivity.
Inflammation happens as the body sends white blood cells and healing nutrients to the areabut too much swelling can limit mobility and slow healing.
A physiotherapist works to balance healing with gentle activity so your body recovers efficientlywithout complications like stiffness, scar tissue, or chronic pain.
??? How Physiotherapy Helps with Post-Surgical Pain and Inflammation
1. Early Mobilization
One of the most important (and safest!) strategies is to start movinggentlyearly.
This improves circulation, reduces swelling, and prevents stiffness.
It also reduces the risk of post-surgical complications like blood clots or joint contractures.
Your physio will guide you through pain-free, low-impact movements tailored to your surgery typewhether its a joint replacement, tendon repair, or abdominal procedure.
2. Manual Therapy Techniques
Hands-on techniques help ease pain and reduce inflammation, such as:
Gentle massage and lymphatic drainage to clear swelling
Scar tissue mobilization to prevent adhesions
Passive range-of-motion exercises to restore flexibility and comfort
These techniques also help retrain muscles and joints to move normally again.
3. Pain-Relief Modalities
Physiotherapists often use tools and techniques to calm down post-op pain and swelling:
TENS (electrical stimulation) to block pain signals
Cold therapy (cryotherapy) to reduce inflammation
Heat therapy (for later stages) to improve mobility
Ultrasound therapy to promote soft tissue healing
Taping techniques to support muscles and reduce swelling
All are carefully timed and dosed to match your stage of healing.
4. Exercise Prescription
Movement is medicinewhen done right. Your physio will design a personalized rehab program that includes:
Gentle strengthening of nearby muscles without stressing the surgical site
Controlled stretching to avoid joint or muscle tightness
Gradual load progression to rebuild stability and strength over time
These exercises are introduced in phases to match your healing timeline, and they evolve as you get stronger.
5. Education & Empowerment
Your physio doesnt just treatyoull also learn:
How to move safely and confidently (getting out of bed, walking, lifting, etc.)
What to avoid that might worsen swelling or delay healing
How to manage pain at home with positioning, pacing, and ice/heat strategies
When and how to return to daily activities, work, or exercise
Knowledge = less fear, more control, and a smoother recovery journey.
6. Preventing Chronic Pain
Untreated post-op pain can become chronic if:
Nerves become hypersensitive
Muscles stiffen or weaken
The brain develops pain-memory patterns
Physiotherapy keeps pain functional and short-term, by helping the body move confidently through recovery milestones. Thats why early rehab is so important.
?? How Long Will Recovery Take?
It depends on the type of surgery, but generally:
Minor procedures: 26 weeks
Joint replacements: 612+ weeks
Soft tissue repairs (like ACL, rotator cuff): 36 months (or more)
But heres the key: physio shortens recovery time, improves outcomes, and reduces the chances of long-term pain or complications.
? Final Takeaway
Physiotherapists are essential allies in your post-surgery journey. They dont just treat painthey help you understand it, reduce it naturally, and move beyond it with confidence. Whether youre recovering from a joint replacement, fracture, or soft tissue repair, physio helps you heal faster, with less pain and better long-term function.